Understanding Blood Sugar: The Foundation for Weight Loss After 40
How to work with your body instead of fighting it. The truth about carbs, sugar spikes, and why understanding this one system makes weight loss easier.
You eat porridge with berries for breakfast with a glass of orange juice. Healthy choice, right? By 10 AM you’re standing in the kitchen, trying to decide if you’re actually hungry or if you should just power through. You tell yourself you’ll wait until lunch.
You don’t make it. By 11:30 you’ve eaten three things you didn’t plan on and you’re annoyed with yourself.
Lunch is a sandwich and an apple. Solid meal. Then 2:30 hits and you’re fighting to keep your eyes open. You need coffee. And something sweet. Just to get through the afternoon.
If this sounds familiar, it’s important to know it’s not a personal failure. This isn’t about lack of willpower, being addicted to food or sugar. This very likely has to do with your blood sugar running the show, and you can transform how you feel and how your day goes, by understanding how your body works and working with it.
If you’re over 40 and struggling to lose weight despite doing “everything right,” understanding blood sugar might be the missing piece. Not because you need another set of rules to follow, but because once you understand how this system works, it can make everything else - what you eat, how much you eat, when you eat - so much easier to do.
What Is Blood Sugar
Your blood sugar is the amount of glucose (a type of sugar) circulating in your bloodstream at any moment. Glucose is your body’s primary fuel source. Your brain runs almost exclusively on it, using about 120 grams a day. Your muscles use it for movement. Every cell in your body needs it to produce energy.
We all need glucose. It’s essential. The problem starts when the amount of glucose in our bloodstream swings wildly up and down throughout the day.
Here’s how it’s supposed to work:
You eat food that contains carbohydrates. During digestion, those carbohydrates break down into glucose, which enters your bloodstream. Your blood sugar level rises - a normal and necessary phenomenon. You shouldn’t be scared of ‘sugar spikes’ after eating carbs; if your blood sugar doesn’t go up after eating, something isn’t working as it should. Once your pancreas detects this rise in blood sugar levels, it releases insulin, a hormone that acts like a key. Insulin unlocks your cells, allowing glucose to move from your bloodstream into your cells where it can be used for energy. As glucose moves out of your bloodstream and into your cells, your blood sugar level comes back down.
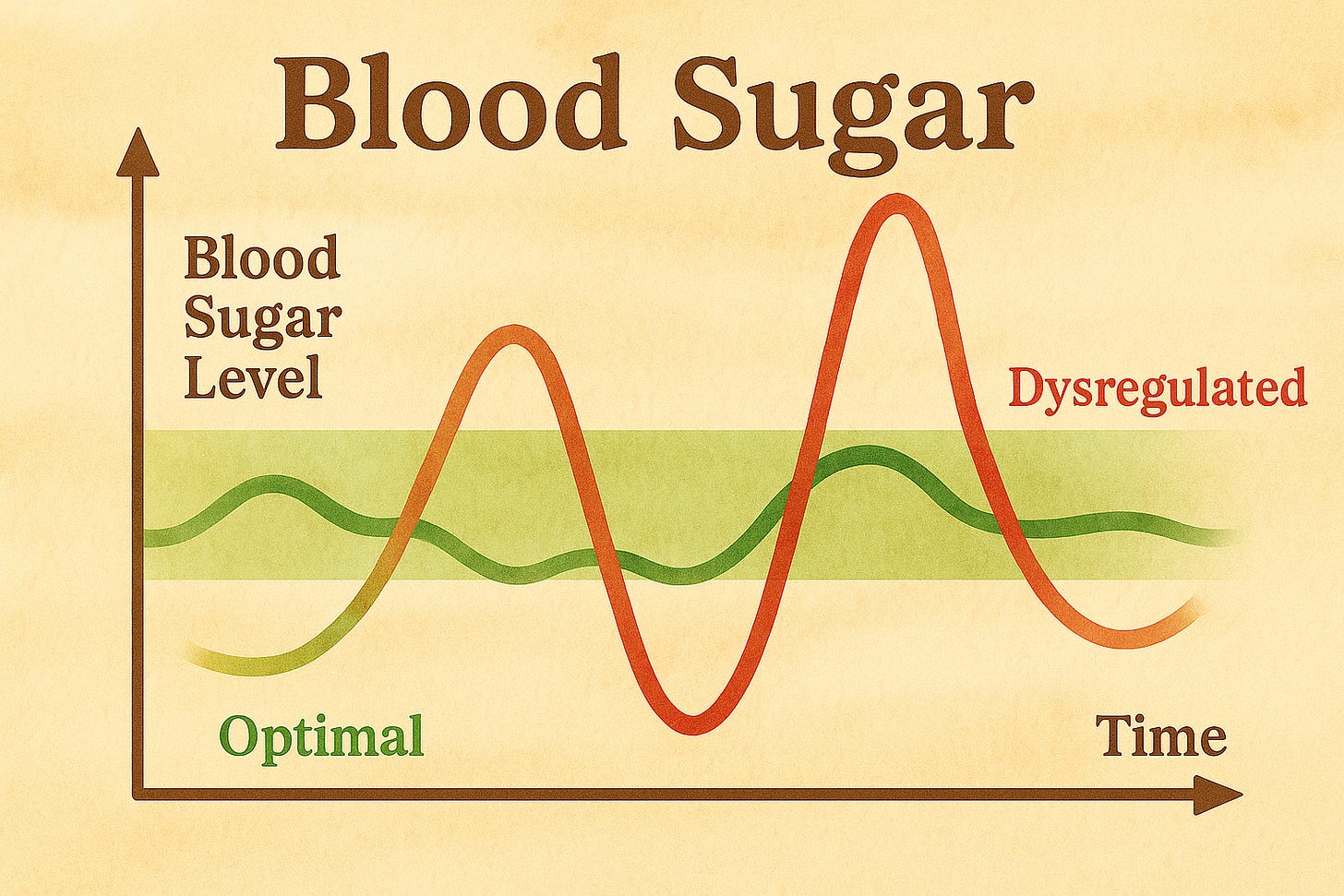
When everything works as it should, this happens smoothly. Blood sugar rises gently after eating, then comes back down to baseline over the next few hours. You feel satisfied after eating and comfortably hungry before your next meal. Your energy stays relatively stable. Your brain works clearly.
If you’ve ever used a CGM (continuous glucose monitor) that measures blood sugar levels, the normal range for blood sugar is roughly 3.9-5.6 mmol/L (70-100 mg/dL) when you haven’t eaten (fasting), and ideally it shouldn’t spike much above 7.8 mmol/L (140 mg/dL) even after a meal (though this differs between different people and the fact that it sometimes climbs higher doesn’t make you unhealthy). These are more or less the ranges. Your body works hard to keep blood sugar levels in this range because both high and low blood sugar can create problems.
But for many women, especially those over 40, this system has stopped working smoothly. Instead of gentle rises and falls, blood sugar is spiking high and crashing low multiple times a day. The result is constant hunger, energy crashes, brain fog, and a body that’s stuck in fat-storage mode.
The Spike-Crash Cycle (And Why You Can’t Stop Thinking About Food)
When blood sugar is dysregulated, it affects your hunger levels, your cravings, your energy levels and how clear headed and sharp you feel.
Let’s use the original eating scenario from the beginning of the post to understand how this works.
The Morning Spike: You eat a bowl of porridge with berries, accompanied by some orange juice. Porridge is mostly carbohydrate, a very healthy carbohydrate, but you’re eating it with minimal protein or fat to slow digestion. The orange juice is mostly sugar: no fibre left from the oranges, just distilled sugar and water. Within 30-45 minutes, that porridge has broken down into glucose and entered your bloodstream rapidly, along with the sugar from the orange juice. Your blood sugar shoots up.
Your pancreas detects this spike and responds by releasing a surge of insulin into your bloodstream. Insulin’s job is to get that glucose out of your blood and into your cells quickly. And it does its job - maybe too well.
The Morning Crash: By 10 AM, all that insulin has driven your blood sugar back down. But because the spike was so high and so fast, your body may have overcompensated. Now your blood sugar is sitting below baseline, let’s say at 3.6-3.9 mmol/L (65-70 mg/dL). That’s not dangerously low, but it’s low enough that your brain, which runs on glucose and is very sensitive to energy availability, starts sounding alarms.
You feel tired. You can’t concentrate. And you feel hungry even though you just ate two hours ago.
This isn’t psychological. This is your brain running low on its primary fuel source. It’s responding by releasing hunger hormones, specifically ghrelin, which signals “you need to eat NOW”, whilst suppressing leptin, the hormone that tells you you’re satisfied. Remember, your brain is always geared towards survival. If it perceives energy sources as low because blood sugar levels are down, it will do what it needs to do to make sure you quickly provide it with more energy - it will make you hungry.
It will also trigger your body to release stress hormones (cortisol and adrenaline) to bring blood sugar back up by signalling your liver to release stored glucose. This is an emergency response system designed to keep you alive. When the body is worried not enough energy is coming in, it starts a process that releases glucose to the blood from the liver (glycogenolysis), basically saying - not enough is coming in, let’s make some ourselves. As a result you might feel slightly jittery or anxious alongside the hunger.
Your body is pressing the brake pedal and the gas pedal simultaneously, whatever is needed to get energy into your cells. It doesn’t care or understand that there’s lots of energy padding your body in the form of fat. All it knows is that blood sugar crashed, and we need to get some energy in pronto.
You’re back in the kitchen: You give in and eat something - maybe a cereal bar or a few handfuls of biscuits. More refined carbohydrates. Your blood sugar spikes again, insulin floods your system again, and two hours later you crash again.
By the afternoon, you’ve been on this rollercoaster three or four times. Your pancreas has been releasing insulin all day. Your hunger hormones are confused. Your stress hormones are elevated. And you’re standing in front of the cupboard at 8 PM eating crackers, chocolate or whatever else, whilst telling yourself you have no willpower.
But willpower has nothing to do with it. You’ve spent the entire day in a biochemical cycle that creates real, physical hunger every few hours.
The Second Meal Effect
How you start the day matters more than you think. What you eat for breakfast doesn’t just affect your morning - it sets up your blood sugar response for the entire day. It’s called the “second meal effect” and has been studied extensively.
When you start your day with a high-carb, high-sugar breakfast (think pastries, sugary cereal, or juice), you trigger that spike-crash cycle. But what makes it worse is that the initial crash makes your body more reactive to carbohydrates at your next meal. Your lunch, even if it’s relatively balanced, will cause a bigger blood sugar spike than it would have if you’d eaten a more balanced meal for breakfast. The result is more insulin, another crash, more cravings.
If you start your day with the wrong meal, you spend the whole day chasing blood sugar stability but never catching it. You’re hungrier at every meal, your cravings are stronger, and by evening you’re standing in front of the fridge convinced you have no self-control. But what’s really happening is that you’ve set a biochemical cascade at 7 AM that’s been running all day. If you’ve ever felt like once you’ve started the day eating ‘badly’, the whole day is ruined, this is part of the reason.
High Insulin Keeps You From Burning Fat
Increased hunger and constant eating aren’t the only things driving your weight gain or preventing weight loss. Insulin not only opens cells up to take on glucose and convert it to energy, it’s also the master storage hormone in our body.
When insulin is present in the bloodstream - which happens every single time you eat - and when it stays elevated because you’re on the blood sugar rollercoaster (eating and crashing, eating again and crashing again), it sends your body a clear message: store energy, don’t burn it. And where does it store that energy? You guessed it. Fat.
Insulin does this by controlling specific enzymes. Think of these enzymes like switches that turn fat storage on or fat burning on. When insulin is elevated, it flips the switches to storage mode. The enzyme that pulls fat out of storage and breaks it down (hormone-sensitive lipase) is turned off. The enzyme that pulls fat into storage cells (lipoprotein lipase) is turned on.
Now, If you’re eating fewer calories than your body needs, you will still lose weight. The laws of physics don’t stop working. But when insulin is chronically elevated from blood sugar chaos, your body struggles to access stored fat efficiently for that energy deficit. You’re walking around with stored energy in your fat cells, but the hormonal environment won’t let you use it easily.
Instead, when you’re in a calorie deficit with chronically high insulin, your body is more likely to break down muscle tissue for energy. The ratio of muscle loss to fat loss shifts towards more muscle loss. This is why so many women feel terrible when they try to lose weight by just eating less and moving more: tired, weak, cold, irritable. They’re not accessing their fat stores efficiently. They’re losing muscle, which then slows their metabolism further, making weight loss even harder and weight regain far more likely.
The answer beyond balancing your blood sugar is to build muscle, through resistance training and to consume adequate amounts of protein. Research shows that those probably matter more to the ratio of fat:muscle loss than any effects from higher insulin (and building muscle will also help increase your insulin sensitivity).
We’ll cover how to make your blood sugar stay stable in a minute, but for now it’s important to understand that the more stable your blood sugar is, the lower, more stable insulin levels you’ll have, which means your body can actually access stored fat when you need energy, which translates to fat loss.
Why You Should Care: The Cost of Blood Sugar Dysregulation
If you’re not convinced yet, let me call out the impact unstable blood sugar has on your daily life, because it’s more than you probably realise and goes way beyond weight and looks.
Your energy levels: That 3 PM slump isn’t normal ageing and it’s not because you need more coffee. It’s very likely your blood sugar bottoming out after a lunchtime spike. Your brain is literally running on inadequate fuel because blood sugar crashed after spiking. The fatigue is real and physical, not psychological.
Your constant hunger: When your blood sugar crashes, your body releases ghrelin (the hunger hormone) and suppresses leptin (the satiety hormone). You feel genuinely, physically hungry even if you ate recently. You’re not weak or lacking discipline. Your hunger hormones are responding to actual blood sugar levels.
Your cravings: When blood sugar crashes, your body wants quick energy to bring it back up. That’s why you crave sweet things and specifically refined carbs - they’re the fastest way to raise blood sugar. Your body is trying to fix a problem: not enough sugar, by getting you to eat some more. The solution isn’t discipline or willpower in resisting the cravings. It’s preventing the crash from happening in the first place.
Your ability to burn fat: As I mentioned, chronically high insulin makes it difficult for your body to access stored fat efficiently. If you’re on the blood sugar rollercoaster, insulin stays elevated most of the day. You’re metabolically stuck, unable to use your own stored energy, basically sabotaging your attempts at weight loss.
Your sleep: Blood sugar crashes don’t stop when you’re asleep. If your blood sugar drops too low during the night (maybe after a late night binge), your body releases stress hormones to bring it back up. These hormones can wake you up or prevent deep sleep (hello waking up at 3 AM every night to scroll on your phone, wide awake). In the morning, you wake up tired, which studies show makes blood sugar regulation even worse the next day. It’s a vicious cycle.
Your mood and focus: Your brain needs steady glucose. When blood sugar is all over the place, so is your cognitive function. Brain fog, irritability, difficulty making decisions, forgetting words - these aren’t just menopause symptoms. They’re often the result of blood sugar instability (and they can get worse with hormonal shifts through perimenopause and menopause).
Your stress response: The blood sugar rollercoaster triggers cortisol release throughout the day. Chronic elevated cortisol worsens insulin resistance, promotes belly fat storage, and makes weight loss harder. It also makes you feel anxious and on edge even when nothing is objectively wrong.
Why This Gets Worse After 40
If you’ve noticed that the same eating patterns that worked perfectly fine in your 30s stopped working in your 40s, you’re not imagining it. Your body’s blood sugar regulation system changes significantly during perimenopause and menopause.
The main reason is (as always) declining oestrogen. Oestrogen plays a role in insulin sensitivity - how readily your cells respond to insulin’s signal. As oestrogen drops, your cells become more resistant to insulin.
Think of insulin resistance like this: insulin is still the key trying to unlock your cells, but the lock has got stiff. The key still fits, but it takes more effort to turn. Your pancreas responds by producing more insulin to get the same job done, essentially trying to use more force to open the lock. If your cells now need 5 units of insulin to handle the same amount of glucose they used to handle with 2 units, your pancreas will make 5 units.
This means that after 40, the same meal that used to cause a moderate insulin response now causes a much larger one. And remember, insulin is the storage hormone. More insulin in your system means:
More difficulty accessing stored fat for energy
More likely to store incoming energy as fat
More fat stored specifically around your midsection
At the same time, declining oestrogen affects your hunger hormones directly. Many women notice they feel hungrier more often after 40. This isn’t psychological. Your body is experiencing hormonal changes that increase appetite whilst simultaneously making it harder to burn stored fat.
Sleep disruption from night sweats and hormonal changes can compound the problem. Research shows that poor sleep increases insulin resistance and makes you crave high-carb foods the next day for quick energy.
So you can see how with dysregulated blood sugar, especially in your 40s and beyond, you’re fighting biology on multiple fronts.
Do You Need to Avoid All Carbs and Sugar?
I hope you don’t take away from this that you are better off eliminating carbohydrates from your diet.
Your brain needs about 120 grams of glucose per day to function properly. Your muscles use glucose for energy. Carbohydrates are not the enemy. The issue isn’t carbohydrates. It’s the type of carbohydrates and the context in which you eat them.
Complex carbohydrates - whole grains, legumes, starchy vegetables like sweet potatoes, and fruits - come packaged with fibre, vitamins, minerals, and often protein. That fibre naturally slows down glucose absorption. When you eat a bowl of lentils or a sweet potato, your blood sugar rises gradually and stays stable. These foods also keep you full for hours, support your gut health, and provide nutrients your body needs.
Research consistently shows that diets rich in whole grains and legumes are associated with better blood sugar control, lower risk of type 2 diabetes, and easier weight management. The fibre in these foods does exactly what we want - it blunts the blood sugar spike naturally.
Refined carbohydrates - white bread, pastries, sugary cereals, crisps, biscuits - have had their fibre stripped away during processing. What’s left is quickly broken down into glucose and hits your bloodstream fast. This is what creates the spike-crash rollercoaster. It’s not that these foods are “bad” or “forbidden.” It’s that they lack the natural buffers that make carbohydrates work well in your body.
What about sugar specifically?
Added sugar - the kind in sweets, cakes, fizzy drinks, and many processed foods - is essentially refined carbohydrate in its purest form. It spikes blood sugar quickly and provides no nutritional value beyond energy.
Does that mean you should prioritise eating sugar? Probably not. There is very little nutritional value in doing that. Does this mean you can never have sugar? The answer is no.
We eat for many other reasons than for nutritional value. Joy, pleasure, flavour and socialy to name just some of them. Having a piece of birthday cake, enjoying dessert on a special occasion, or having a biscuit with your tea occasionally isn’t going to derail your health or weight loss. The human body is remarkably resilient. The occasional blood sugar spike doesn’t undo weeks of stable eating.
What matters is the pattern. If you’re eating sugary foods multiple times every day - sweetened coffee drinks, sugary cereal for breakfast, biscuits at morning tea, a fizzy drink with lunch, sweets in the afternoon and chocolate in the evening - your blood sugar is constantly spiking and crashing. That’s when you run into problems with constant hunger, cravings, energy crashes, and difficulty losing weight.
But if most of your carbohydrates come from whole food sources and you have sugar occasionally as a treat? Your body can handle that easily.
The practical approach:
Build most of your meals around whole food carbohydrates - vegetables, fruits, whole grains, legumes. These provide the glucose your body needs along with fibre and nutrients that support stable blood sugar.
When you do eat refined carbohydrates or sugar, do it consciously and ideally alongside protein, fat, or fibre. A biscuit with a cup of tea and some cheese won’t cause the same blood sugar chaos as eating half a chocolate bar on an empty stomach.
The goal is stability and consistency most of the time, not perfection all the time. You don’t need to fear carbohydrates. You need to understand how to eat them in a way that works with your body.
The Good News: There’s A Lot You Can Do to Stabilise Blood Sugar
Here are the foundational strategies. I’ll write more detailed posts later in this series about implementing them, but this is what you need to understand as the baseline.
Carbohydrates like company - Try eating your carbohydrates with protein, fat or fibre. When you eat carbohydrates by themselves - even healthy ones like fruit or porridge - they break down quickly into glucose and hit your bloodstream fast. This creates the spike that starts the whole cycle.
When you pair carbohydrates with protein, fat, or fibre, you slow down digestion. The glucose enters your bloodstream gradually instead of all at once. Your blood sugar rises gently, insulin response is moderate, and you avoid the crash.
Whole foods like apples already contain fibre, which is why eating an apple on its own is generally fine for most people - the fibre in the fruit slows glucose absorption naturally. Where this matters most is with refined carbohydrates that have had their fibre stripped away. Apple juice, for instance, is essentially sugar and water with no fibre to slow absorption - it hits your bloodstream fast and causes the spike-crash cycle. The same is true for white bread, pastries, or sugary cereals.
If you find yourself still hungry or experiencing energy crashes even with whole foods, adding protein or fat can help. An apple with a handful of almonds or some cheese will keep you satisfied longer than the apple alone. But if you eat an apple and feel fine for hours? Your body is handling it well. This isn’t about perfection - it’s about understanding what works for your body and adjusting when needed.
Protein is your anchor at every meal - Protein slows stomach emptying, which means glucose enters your bloodstream more slowly. It also has minimal effect on blood sugar itself - unlike carbohydrates, protein doesn’t cause a spike. Including 25-30 grams of protein at each meal creates stability.
There’s also evidence that higher protein intake improves insulin sensitivity, especially in women over 40. To read more about why protein is non-negotiable, read this post, but for blood sugar stability, it’s essential.
Fibre slows glucose absorption - Fibre is the non-digestible part of plant foods. When you eat fibre alongside carbohydrates, it physically slows down how quickly those carbohydrates break down into glucose. A meal with protein and lots of vegetables will have a completely different blood sugar response than the same protein with white rice.
This is why eating patterns that include lots of non-starchy vegetables (leafy greens, broccoli, peppers, cauliflower, courgette, etc.) alongside protein and moderate amounts of starchy carbs work so well for blood sugar stability. You’re getting volume and nutrients but also slowing glucose absorption. The order of eating matters here - ideally start with the salad or vegetables and protein before moving to carbs.
Fat smooths the curve - Healthy fats such as olive oil, avocado, nuts, seeds, fatty fish, slow stomach emptying even more than protein alone. They create a gradual, sustained release of glucose into your bloodstream. The blood sugar curve is lower and wider instead of a sharp spike and crash.
Fat is calorie-dense though, so you don’t need huge amounts. A tablespoon of olive oil on your salad, a quarter of an avocado, a small handful of nuts - these portions are enough to create the stabilising effect without adding excessive calories.
The breakfast effect matters - What you eat at your first meal sets the tone for your blood sugar regulation for the entire day. Studies show that people who eat high-protein breakfasts have better appetite control, reduced cravings, and more stable blood sugar throughout the day compared to those who eat high-carb breakfasts or skip breakfast entirely.
This doesn’t mean you have to eat the moment you wake up, but within the first hour or two, prioritise protein. Eggs, Greek yoghurt, protein smoothie, even leftovers from dinner. Get 25-30 grams of protein. Notice how you feel at 10 AM compared to after eating a more carb-centric breakfast.
Movement after meals helps - When you move your body, your muscles take up glucose from your bloodstream without needing as much insulin. Even a 10-15 minute walk after eating - especially after dinner - can significantly reduce the blood sugar spike from that meal. Your muscles are literally pulling glucose out of your blood and using it for energy. This is one of the most effective tools you have, and it requires no equipment or gym membership. A short walk after a meal, jumping or squatting in place, even heavy fidgeting will help.
You Don’t Need to Be Perfect
The goal isn’t perfect blood sugar all day every day. That’s not realistic and it’s not necessary. Your blood sugar levels will always spike after eating carbs and sugary foods, sometimes high, and that’s normal and nothing to fight. I love and eat lots of grapes, often on their own. Blood sugar spikes! That’s OK.
The goal is reducing the volatility. Fewer dramatic spikes and crashes. More stability. You’re not trying to keep your blood sugar at 4.7 mmol/L (85 mg/dL) constantly. You’re trying to avoid the spike to 9.4 mmol/L (170 mg/dL) followed by the crash to 3.6 mmol/L (65 mg/dL) that leaves you tired and starving.
This means you don’t have to eliminate carbs or follow complicated rules. You need to understand how to build meals that keep you stable. Sometimes you’ll eat something that causes a spike - birthday cake, a bagel, crisps, some chocolate - whatever. That’s fine. It’s not about never having those foods. It’s about not living on that rollercoaster every single day.
Most women who start focusing on blood sugar stability notice significant changes very quickly:
More stable energy throughout the day
Less hunger between meals
Fewer cravings for sugar and refined carbs
Better sleep
Clearer thinking
And yes, easier weight loss, because their hormones are finally working with them instead of against them
Where Do You Start?
Pick one thing to focus on this week. Not everything. One thing.
Maybe it’s eating a high-protein breakfast every morning and noticing how you feel at 10 AM compared to your usual breakfast.
Maybe it’s adding protein to whatever you’re already eating for lunch and seeing if you make it through the afternoon without the energy crash.
Maybe it’s taking a 10-minute walk after dinner and tracking how you sleep.
One change. Notice what happens. Then add another.
Start observing what stable blood sugar feels like in your body. Once you know what it feels like, you can recreate it. It usually takes only a week of consistency to start noticing changes in how you feel.
In the next couple of posts I’ll touch on other aspects of blood sugar balance. It can impact so many things in our body and our health. From raising inflammation and making your body hold on to fat, to contributing to fat distribution around the belly and sabotaging your weight loss efforts.
But I hope, to start with, this post is a good foundation for what blood sugar is and how it can affect your weight loss journey.
If you have been struggling with weight not moving and feeling like your body is refusing to cooperate, it could just be that imbalanced blood sugar is at fault and you’ve just been trying to manage weight without understanding the hormonal system that controls it.




Thank you for this post. Very interesting! Looking forward to more!!
People have advised me on several occasions to add 500 ml of water to breakfast. Is this just for filling and fluids or does it affect the blood sugar somehow (or does it have an effect on how the foods are processed?)