Belly Fat After 40: Why Perimenopause Changes Where You Store Fat (And What You Can Do About It)
Why it happens, how it's different from regular belly fat, and what you can do about it
You’re eating the same, maybe even less. You’re exercising. But your waist feels like it’s thickening in a way it never did before.
Your jeans don’t fit the same way. Not because you’ve gained a lot of weight - the scale might have barely budged. But everything sits differently now. Tighter around the middle. And when you do gain weight, it accumulates in places it never used to, specifically your belly.
You’re not imagining it. This is what’s sometimes called the “menopause belly” - and it’s a result of a biological shift triggered by hormonal changes in your 40s and 50s. About 65-75% of women over 40 experience it.
The fat isn’t necessarily new - It’s relocating. And understanding the mechanism behind this shift will show you exactly what you can do about it.
What Is the “Menopause Belly”?
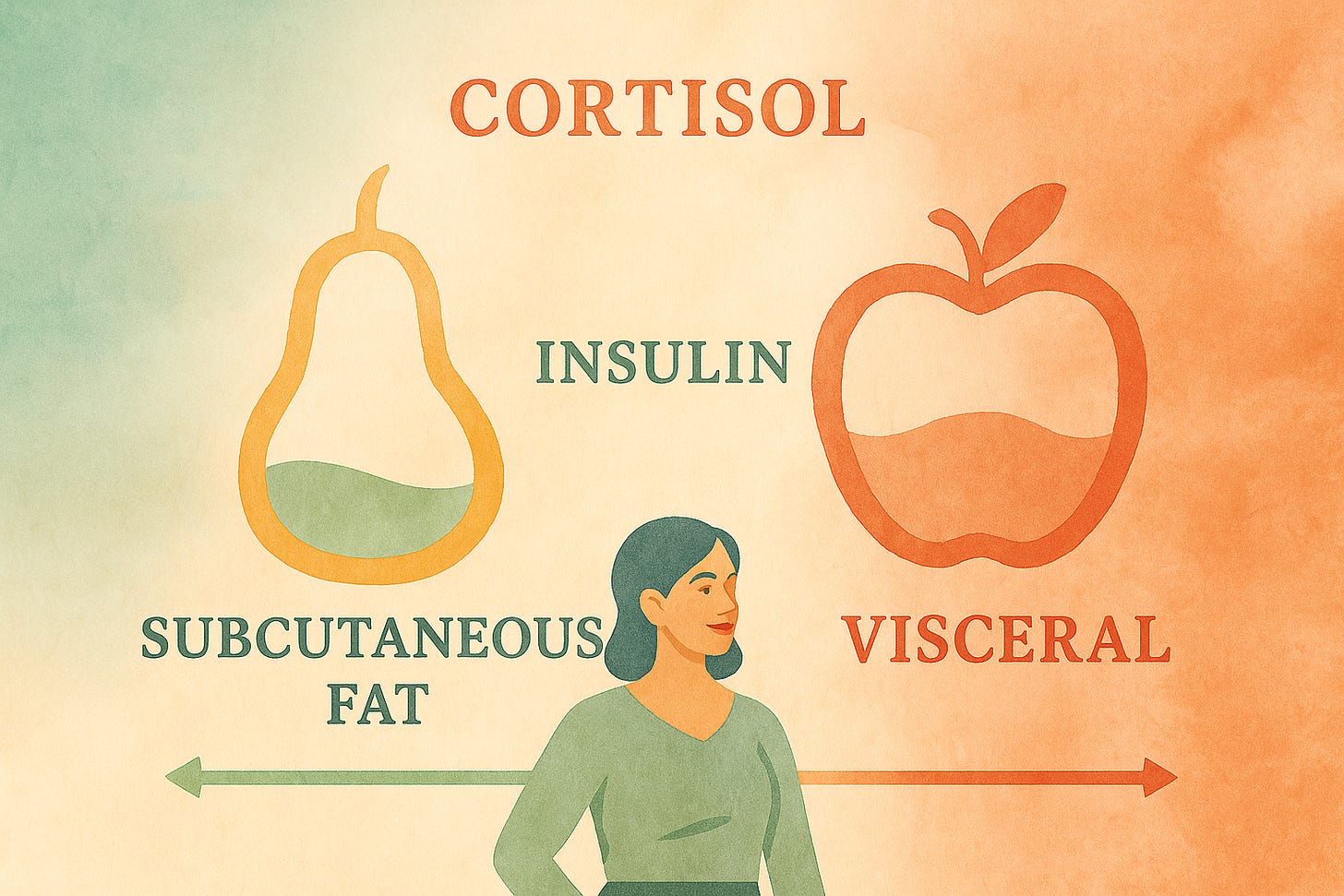
The term Menopause belly isn’t just about weight gain. It’s a specific pattern of fat redistribution that happens when estrogen declines during perimenopause and menopause.
Before this hormonal shift, your body preferentially stored fat in subcutaneous deposits - the soft layer under your skin on your hips, thighs, and arms. This gave you curves and served important metabolic functions: energy storage, insulation from cold, mechanical cushioning (so you won’t break anything if you fall), and helped with leptin secretion (the hormone that signals fullness, the more fat you have, the more leptin is available to signal no additional food is needed).
But when estrogen drops, something fundamental changes. Your body starts directing fat to a different location: deep inside your abdomen, wrapped around your organs. This is called visceral fat, and it behaves completely differently from the subcutaneous fat under your skin.
Studies show that early postmenopausal women gain 36% more fat around the middle and 49% more fat inside the abdomen, compared to their pre menopausal state, even without gaining significant overall weight. As estrogen levels fall, visceral fat increases from 5-8% of body weight to 10-15%.
Your body shifts from pear shape, where fat is accumulated around your butt and hips (cushioning your reproductive organs) to more of an apple shape, around your middle.
And this isn’t just about appearance. That deep visceral fat creates metabolic problems that subcutaneous fat typically doesn’t (at least not until you exceed a certain level).
Not All Belly Fat Is Related to Menopause
Before we go further, let’s be clear about something: not every bit of belly fat is menopause related. If you’re carrying extra weight all over your body, some of that fat will naturally sit on your belly - that’s just normal fat distribution. To reduce it, you’d need to lose weight overall through a calorie deficit. Those sculpted, flat tummies you see come from two things: low overall body fat percentage and strong core muscles (built through exercise that targets the core directly or indirectly). The less fat you have overall, the less fat you have around your middle, the more you see the muscles you do or don’t have - hence a flat (and maybe sculpted tummy).
But the ‘menopause belly’ is different. It’s when you’re not gaining significant weight overall, you’re eating roughly the same as you always have, yet your belly specifically is growing. You might even lose weight elsewhere whilst your middle thickens. This pattern typically emerges in your late 40s onwards, coinciding with hormonal changes. That’s when we suspect the menopause belly phenomenon - not general weight gain, but a specific redistribution of fat to your abdomen driven by declining estrogen.
Two Types of Fat, Two Different Behaviors
We have two main types of fat storage, and they function very differently.
Subcutaneous fat sits just under your skin. It’s the fat you can pinch. In healthy amounts, it’s not problematic - it’s actually part of normal physiology. It’s only when subcutaneous fat tissue becomes overloaded and inflamed, when fat cells enlarge beyond their healthy capacity, that it starts affecting metabolism and health outcomes.
Visceral fat is different from the start. It sits deep in your abdomen, wrapped around your liver, intestines, and stomach. You can’t pinch it because it’s internal. And it’s metabolically active from day one - it doesn’t just store energy quietly. It secretes hormones and inflammatory compounds directly into your bloodstream. It affects how your body processes insulin. It increases your risk for cardiovascular disease and type 2 diabetes.
Before perimenopause, estrogen acts like a traffic director for fat storage. It preferentially sends fat to subcutaneous storage sites and actively protects against visceral fat accumulation.
But when estrogen starts declining in your 40s, that protection disappears.
The fat storage GPS gets reprogrammed. Same amount of fat, different destination.
Three Hormonal Changes Drive Belly Fat in Perimenopause
Three hormonal shifts happen simultaneously during perimenopause, and they all point fat toward your middle.
Threat #1: Declining Estrogen
Estrogen does more than you probably realize for fat metabolism.
It maintains insulin sensitivity - when glucose is available in your blood after a meal, your pancreas secretes insulin to signal cells to take glucose inside and transform it into energy. Insulin sensitivity refers to how readily your cells respond to insulin’s signal.
When estrogen drops, your cells become more resistant to insulin. The key still fits the lock, but the lock has gotten stiff. It takes more effort to turn.
Your pancreas responds by producing more insulin to get the same job done. If your cells now need 5 units of insulin to handle the same glucose they used to handle with 2 units, your pancreas makes 5 units.
More insulin in your system means more fat storage. And visceral fat has more insulin receptors than subcutaneous fat. When insulin levels are high, visceral fat becomes the preferred storage site - hence a bigger belly.
Estrogen decline also accelerates muscle loss. Menopause speeds up the age related decline in muscle mass that happens to everyone (unless you counter it by actively building muscle through training and protein consumption). Lower estrogen means fewer muscle-building signals (like growth hormone and IGF-1) and more muscle breakdown and inflammation.
Less muscle means a slower metabolic rate. Your body burns fewer calories at rest than it used to, making weight gain easier even if you’re eating the same amount.
Estrogen also affects your hunger hormones. Research shows that menopause blunts leptin (which signals satiety) and raises ghrelin (which signals hunger), especially when sleep is poor.
Many women notice they feel hungrier more often after 40. This isn’t psychological. Your body is experiencing real hormonal changes that increase appetite.
Threat #2: Rising Insulin
This is where everything connects back to blood sugar.
Insulin is your master storage hormone. When insulin is present in your bloodstream, it does three things:
It activates fat storage - Insulin turns on the enzyme (lipoprotein lipase) that pulls fatty acids from your bloodstream into fat cells for storage. It also activates the enzymes that convert glucose directly to fat.
It blocks fat burning - When insulin is elevated, it turns off hormone-sensitive lipase - the enzyme that breaks down stored fat. This is the key point: when insulin is high, your body physically cannot access stored fat for energy. You’re locked out of your own reserves.
It signals “fed state” - High insulin tells your body: we have plenty of energy coming in right now, store everything, don’t burn reserves.
Now add insulin resistance to this picture.
With insulin resistance, your pancreas has to make more insulin to do the same job. So insulin levels stay elevated longer throughout the day. And visceral fat (that deep belly fat around your organs) has more insulin receptors than any other fat tissue in your body. It’s more metabolically active and more responsive to hormonal signals.
The result: high insulin + loss of estrogen’s protective effect = more fat storage in the belly.
And here’s where it compounds: Visceral fat doesn’t just sit there. It releases inflammatory compounds into your bloodstream. These inflammatory signals make insulin resistance worse. Which means your pancreas makes even more insulin. Which stores more belly fat. Which releases more inflammation.
Insulin resistance drives belly fat, and belly fat worsens insulin resistance.
Threat #3: Elevated Cortisol
Cortisol is your stress hormone, and visceral fat has many cortisol receptors.
Perimenopause is often a stressful time. Sleep disruption from night sweats and hormonal changes is common. Life stress like caring for aging parents, teenagers at home, career demands, often peaks for women in their 40s and 50s.
When cortisol is chronically high, it does two things that worsen belly fat: it encourages fat storage, particularly in the abdomen where there are more cortisol receptors. And it increases appetite, especially for high-sugar, high-fat comfort foods.
High cortisol + high insulin + low estrogen = a perfect storm for belly fat accumulation.
Which is why women in perimenopause often gain weight specifically around their middle, even when their overall weight doesn’t change much.
Why Visceral Fat Matters More Than Just Aesthetics
This isn’t just about how you look. Visceral fat is metabolically dangerous in ways that moderate amounts of subcutaneous fat aren’t.
Visceral fat behaves more like an active endocrine organ than a storage depot. It secretes inflammatory compounds directly into your bloodstream. These compounds create chronic low-grade inflammation throughout your body.
This inflammation worsens insulin resistance, creating that vicious cycle. It increases your risk for cardiovascular disease. It raises your chances of developing type 2 diabetes and metabolic syndrome.
After menopause, studies show that fat cells in both subcutaneous and visceral depots enlarge, and the tissue shows more inflammation and scarring. The fat tissue itself can become dysfunctional.
This is why some doctors ask about your waist circumference. It’s not about aesthetics. Waist measurement is a health marker - a proxy for how much visceral fat you’re carrying.
What You Can Control
You can’t stop estrogen from declining. That’s menopause, and it’s going to happen.
But you can control the other two hormones in this equation. You can manage insulin through how you eat. You can manage cortisol through how you handle stress and prioritize sleep. And you can build muscle through strength training, which directly attacks insulin resistance.
These aren’t small interventions. Research on postmenopausal women shows that lifestyle changes can substantially reduce visceral fat and improve metabolic health.
Strategy #1: Stabilize Blood Sugar to Lower Insulin
The most powerful intervention for belly fat is controlling insulin through blood sugar stability.
When you eat foods that spike blood sugar quickly (refined carbs, sugary foods, even just carbs without protein or fat), your pancreas floods your system with insulin. High insulin = fat storage mode, particularly in visceral depots.
When you stabilize blood sugar by pairing protein with every meal and avoiding naked carbs, insulin stays lower and steadier. Lower insulin = your body can actually access stored fat for energy instead of constantly storing more.
Practical application:
- Try not to eat carbs alone. Pair them with protein, fat, or fiber.
- Start meals with protein to blunt the blood sugar response.
- Choose whole food carbs over refined ones when possible.
- Eat at regular intervals to avoid blood sugar crashes that trigger overeating.
Strategy #2: Move After Meals
This is one of the simplest interventions with the biggest impact specifically on belly fat.
When you move after eating (even just a 10 minute walk), your muscles take up glucose from your bloodstream without needing as much insulin. Movement increases glucose uptake directly. This reduces the insulin spike that would otherwise occur after your meal.
Lower insulin spike = less fat storage = less fat stored preferentially in your belly.
You don’t need to run or do an intense aerobic activity. A casual walk around the block works. Even standing and doing dishes or tidying up helps. Anything that gets your muscles contracting and using glucose.
Strategy #3: Build Muscle Through Strength Training
This might be the most important intervention for perimenopausal belly fat, and the research backs it up.
A 15-week supervised resistance training program (3 times per week) in postmenopausal women caused significantly greater losses in visceral and abdominal fat compared to women who didn’t do structured exercise. Even when the scale moved slowly, women who did consistent strength training saw meaningful body composition changes - less belly fat, more muscle.
Here’s why this works so well:
Muscle tissue is metabolically active. It burns calories at rest. More muscle = higher metabolic rate, which counteracts the natural slowing that happens with age and estrogen loss.
Muscle improves insulin sensitivity dramatically. When you have more muscle mass, your body handles glucose better with less insulin. This directly counters the insulin resistance cycle that drives belly fat.
Strength training sends a clear signal to your body: keep this muscle, we need it (to handle the demands placed on our body during training). During perimenopause when your body naturally wants to shed muscle, strength training fights that biological program.
You don’t need to become a bodybuilder. Aim for 2-3 days per week of resistance work. This could be:
- Weight machines at the gym
- Free weights at home
- Bodyweight exercises (push-ups, squats, lunges)
- Resistance bands
- Heavy gardening or similar functional activities
Studies comparing different types of exercise found that combining aerobic exercise (like walking or cycling) with resistance training produced more fat loss and greater lean mass gains than either alone. Do both if you can, but if you’re choosing one, choose strength training for belly fat.
Strategy #4: Cardio for Calorie Burn
Aerobic exercise burns calories and directly reduces abdominal fat. Consistent aerobic workouts, even something as simple as daily brisk walks, have been shown to lead to measurable reductions in visceral fat.
Research shows that more exercise yields more fat loss. Women who exceeded the basic minimum (doing more than 250 minutes per week) saw accelerated belly fat loss.
You don’t need to love running or take intense spinning classes. Find movement you enjoy. The best exercise is the one you’ll do consistently.
Strategy #5: Manage Stress and Cortisol
Chronic stress floods your body with cortisol, which encourages abdominal fat storage and increases appetite for sugary, high-fat foods.
You cannot eliminate stress from your life. But you can change how your body responds to it.
Even 10 minutes daily of intentional stress management helps: walking in nature, deep breathing exercises, meditation, yoga, time on your own with a cup of tea, reading - whatever genuinely calms you. This isn’t optional self-care fluff. It’s hormone management that directly affects where your body stores fat.
Poor sleep also raises cortisol. Night sweats and hormonal changes make sleep disruption common in perimenopause, but finding a way to improve sleep is really important. Aim for 7-8 hours of quality sleep every night. The sleep debt you’re accumulating is directly contributing to belly fat.
Strategy #6: Balance Your Calories
You still need to be in a calorie deficit to lose fat. Nothing bypasses that fundamental truth.
But the quality of those calories matters for where the fat you lose comes from and whether you can sustain the change.
Fill half your plate with vegetables, a quarter with protein, and a quarter with whole carbs or healthy fats. Emphasise a variety of plant-based foods, lean proteins (chicken, fish, legumes, tofu), and healthy fats (olive oil, nuts, avocado). Limit sugary drinks, sweets, saturated fats and processed foods and you will trim belly fat as part of reduced fat everywhere.
Alcohol has also been shown to encourage abdominal fat storage.
Can You Spot Reduce Belly Fat?
Let’s be realistic about what’s possible.
You cannot spot reduce belly fat. No amount of sit-ups or planks will specifically target visceral fat. That’s not how fat loss works.
But when you create the right hormonal environment through the strategies above, belly fat often comes off first.
Why? Because visceral fat is more metabolically active than subcutaneous fat. It responds to hormonal and lifestyle changes faster. When insulin drops and stays low, when cortisol is managed, when you’re building muscle - visceral fat mobilises more easily.
Most women who consistently implement these strategies notice changes within 2-4 weeks. Not a dramatic transformation, but their clothes fit differently around the middle. They have more energy. The bloating reduces.
Within 2-3 months of consistent effort, the changes become visible. Studies show that women who maintained even a 3-5% weight loss kept their visceral fat low. It’s not about losing massive amounts of weight. It’s about changing your body composition.
Some of the belly expansion in perimenopause is inflammation and bloating, not just fat. As your eating improves and inflammation reduces, you might see your waist measurement drop before the scale moves much.
A Reality Check
The bad news: without intervention, this shift tends to persist. The excess visceral fat doesn’t vanish on its own.
Studies tracking women through menopause found that those who remained active and adopted healthier eating fared much better than those who didn’t. Even very fit women saw some fat redistribution - but active women entering menopause had lower BMI, less total and visceral fat, and more muscle than inactive women.
The good news: excess visceral fat can be reduced through deliberate lifestyle changes. Studies on postmenopausal women prove this repeatedly. A combination of smart eating, regular aerobic exercise, strength training, stress management, and adequate sleep works.
You’re not fighting a battle you can’t win. But you do have to engage. The default trajectory without intervention is more belly fat over time. And since these changes benefit not just aesthetics but health, longevity, and how you feel and function, they’re worth the effort.
The belly fat shift is real. It’s driven by biology - specifically by three hormonal changes happening simultaneously in your 40s and 50s. Declining estrogen, rising insulin, elevated cortisol.
You can’t control estrogen decline. That’s biology.
But you can control insulin through how you eat. You can control cortisol through stress management and sleep. You can build muscle through strength training, which attacks insulin resistance at its root.
Three levers you can pull. Three ways to change the hormonal environment that directs fat to your middle.
Women who implement these strategies see real results: less belly fat, better metabolic markers, lower disease risk, more energy, better quality of life.
Your body isn’t working against you. It’s responding to hormonal signals. Change the signals, change the response.